The medical billing process in the healthcare industry is a heavy-duty job that involves a plethora of complex data on medical records, patient information, insurance claims, etc. All of these processes involve a mountain of paperwork and complexities for healthcare professionals and staff. Errors in medical billing management can cause devastating consequences for the healthcare organization and adversely affect overall profitability.
Owing to the difficulties associated with the healthcare billing system, in 1991, the Workgroup for Electronic Data Interchange (WEDI) was introduced into the healthcare system. This development was intended to address the billing challenges health facilities face, improve workflow processes, and reduce overall expenses. Consequently, in 1996, the Health Insurance Portability and Accountability Act (HIPAA) was established for secure EDI billing. HIPAA compliance is a means to secure health data from breaches and maintain privacy.
Why is EDI Essential Today?
Electronic Data Interchange billing is an electronic billing method that uses advanced technology to share data and other related information with standard protocols. Medical EDI is considered the most efficient and reliable means for electronic data exchange relevant to medical claims processing and other billing communication. The privacy of electronic health records is maintained through medical records management, and communication is limited to taking place only between healthcare entities. EDI medical billing software offers healthcare provider solutions designed to provide dynamic solutions that address billing pain points concerning claims, reimbursements, eligibility, and inquiries. Healthcare organizations stand to gain a considerable edge by adopting custom healthcare solutions and healthcare automation with EDI in medical billing.
Role of EDI In Healthcare

EDI transactions are revolutionizing healthcare operations by streamlining administrative processes, reducing costs, and enhancing patient care. They automate tasks like patient registration, claims processing, and invoicing, leading to reduced paperwork and errors. This allows healthcare professionals to focus entirely on improving patient care outcomes, reducing administrative costs, and increasing overall efficiency. EDI transactions also expedite reimbursement processes by submitting claims electronically, reducing the time it takes for claims to be processed and paid. This improves cash flow and financial stability, allowing healthcare providers to invest more resources in patient care.
EDI transactions also enhance patient care by allowing healthcare providers to access confidential patient data in real time. This real-time access facilitates collaboration among healthcare professionals, leading to more meticulous diagnoses and timely interventions. ensuring comprehensive care.
Moreover, EDI transactions enable proactive care management strategies by analyzing patient data to identify trends and patterns. This leads to early disease detection, improved disease management, and better patient outcomes. Overall, EDI transactions play a crucial role in healthcare operations.
EDI Billing and HIPAA
HIPAA is the recognized and authorized protocol that supports the submission and processing of insurance claims analytics. It works as a security blanket for the exchange of health data among different healthcare management entities. The establishment of HIPAA eradicated discrepancies in billing communication and created universal compliance for secure data processing and transmission.
The details of HIPAA are as follows:
- The HIPAA Privacy Rule — To protect patient information
- The HIPAA Security Rule — To protect patient data security
- The HIPAA Enforcement Rule — To set guidelines for HIPAA violations
The Workings of EDI Electronic Billing

EDI Mapping: Incorporating mapping into the EDI billing integration software offers the mapping process to standard EDI documents, along with HIPAA compliant solutions, toward the healthcare billing process. All regular billing records are transferred into EDI formats through cloud computing in healthcare. Turning regular health and billing data into EDI formats ensures the security of sensitive data since these formats are not directly readable. The mapping process seamlessly moves the documents between multiple healthcare entities through integrated healthcare systems.
B2B Transfer: Transmission of EDI billing files, according to HIPAA rules, is undertaken in an encrypted fashion. These comprehensively secure files are then exchanged between parties through a Managed File Transfer (MFT) platform. Under the EDI system, files are transferred through healthcare interoperability and healthcare analytics solutions on this MFT platform. Healthcare providers can send these files to payers, insurance agencies, and pharmacies, and vice versa. Several secure networks for electronic data interchange in healthcare, such as AS2, SFTP, MLLP, etc.
Testing and Validation: Next in line in the EDI system is the validation of the relevant documents. This step requires rigorous testing of EDI in healthcare. Healthcare data is usually sensitive data, and therefore, the testing and validation of data at every level are crucial in EDI healthcare. There are multiple verification steps involved in the testing and validation phase of electronic documents. Every step should be incorporated within the EDI solutions. Just as clinical data analysis uses health data for meaningful purposes, EDI solutions are designed to use medical data for billing purposes.
Integration: Integrated EDI systems use these encrypted documents for multiple billing purposes through integrated care management. Once the healthcare recipients receive the documents, they are translated into usable business formats for various purposes, such as insurance verifications, accounting, healthcare administration, etc. Like how health data is applied toward mHealth and population health management, integrated EDI systems can use data to meet financial requirements.
Features to Look Out For in Healthcare EDI Solutions
Electronic Claims Management
Handling the workflows associated with claims can consume a significant portion of the staff’s time and energy at a healthcare organization. Everything from data entry, claims submission, and claims tracking, coupled with reconciliation, is highly cumbersome and prone to errors. In light of this, EDI claims processing software and medical billing software must have features for managing claims.
The EDI claims management feature must include denial management, claim status monitoring, claims scrubbing, and claim assessment. These functions will streamline the overall process of adjudicating claims and accelerate associated workflows significantly.
Medical Coding
Medical coding involves translating all the billable medical services rendered to patients into standardized ICD codes. This helps provider organizations generate the claims to be sent to payers for reimbursement. An EDI healthcare software with a medical coding feature would accelerate the process and prevent errors. Research has estimated that coding errors cost providers hundreds of millions yearly. However, a coding feature in an EDI system helps minimize coding errors and results in better revenue cycles for providers.
Reporting
The entire healthcare billing process includes several interlinked processes and workflows. Needless to say, the whole process generates large amounts of operational data. Analyzing this data highlights the main causes of denials, rejections, accounts receivables, and problems in coding processes, among others. The insights from the analysis help provider organizations implement corrective measures to address pain points and maximize operational efficiency.
Eligibility Verification
Verifying patients’ health plans is one of the first steps in the overall care process. It ensures that the person’s insurance plan covers the medical services that will be provided and the out-of-pocket expenses to be paid by the patient. This is an important feature for any medical billing management software platform.
A feature for verifying patients’ eligibility considers coverage, co-pays, benefits, deductibles, and others to ensure that the payers can reimburse medical services. This feature reduces claim denials and rejections and improves revenues for providers.
User-Friendly Interface
This rule of thumb applies to all types of software, medical or otherwise. When it comes to medical billing, a user-friendly UI/UX makes the platform navigable and directly impacts working efficiency. Additionally, it would reduce the time needed to train the staff at the organization where it’s implemented, not to mention easing day-to-day medical billing workflows. It is recommended that medical executives view a demonstration of the EDI medical billing solutions to ensure that the staff can work seamlessly with it.
HIPAA Compliance
Data security is a must for any type of software platform that handles patients’ confidential data. In light of this, an EDI billing systems platform must comply with HIPAA (Health Insurance Portability and Accountability Act) regulations. This ensures the software has a certain minimum level of data security features stipulated by government regulation. A HIPAA-compliant solution would ensure that patients’ sensitive data won’t suffer leakage or be compromised in any way.
Custom Developed Vs. Pre-Built
Although this is not a feature of the software, it is a major consideration when choosing medical billing software. Custom-developed software will be designed according to an organization’s requirements. The company developing the application would thoroughly analyze the requirements before deciding on the features and functions. Moreover, it would also reflect the existing mode of operations and workflows, enabling the staff to get acquainted with it faster. However, on the flip side, it would take more time and money than pre-built EDI solutions. A pre-built EDI billing systems platform would be ready to be deployed on an organization’s systems. But However, it would contain a general set of features typical of EDI systems in healthcare. The organization opting for a pre-built solution would have to adjust its workflows accordingly and spend time getting its staff acquainted. On the positive side, this type of software costs less.
Advantages of Electronic Data Interchange Software:
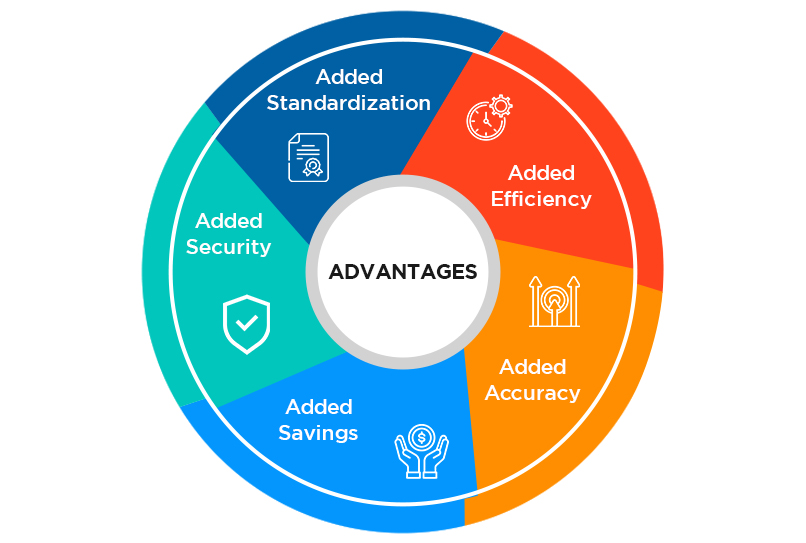
1. Added Efficiency: Electronic data solutions, much like patient engagement solutions, rely on advanced technological features to offer automated processes in billing. There is little room for manual error with secure and precise data exchange, and billing workflows are seamlessly processed. Regular testing and validation, along with compliance protocols, regulates smooth billing and ensures timely completion. Thus, the whole medical billing process is undertaken with optimum efficiency. Finally, ensuring that the solutions are on a cloud-based platform means that data loss is no longer a concern. Agility and accessibility of data is a critical accomplishment within this domain. With enhanced efficiency in medical billing practices, the healthcare organization can immediately expect higher profitability.
2. Added Accuracy: Medical billing is a highly cumbersome process. When undertaken manually, it is prone to increased errors that bring in significant repercussions. The overall process of medical claims involves back and forth between the customer and insurance companies and is quite cumbersome. Paper-based processes and a general lack of technology innovation have hampered the process of claims management. There are volumes of data available, but the lack of structure makes this data unusable. An automated electronic data interchange billing system offers first-rate billing management software through a reliable and secure platform that connects insurance payers, health providers, and patients. It can be created to provide multi-access channels, instant claims checks, and validation in a fully automated and paperless environment.
3. Added Savings: Returned claims with errors, denied claims, rejected bills, incorrect coding, and insufficient data are just a few of the many woes faced by medical billers. Almost 30% of medical bills are prone to medical billing errors. As medical billing and coding errors increase in frequency, patient experience is diminished, profits are adversely affected, and the overall revenue cycle for healthcare is shunted. Efficiently adhering to EDI in healthcare processes and procedures can evade these outcomes through accurate claims management offered through medical billing software. An automated medical billing may be the answer to your healthcare billing and coding needs for increased savings. When systems are prone to human error, the wisest option is to deploy medical billing software embedded with ICD-10 coding solutions and one that is HIPAA compliant.
4. Added Security: Another trigger for medical billing errors is inaccurate and insufficient data collection and usage. Common medical billing mistakes occur when patient information is not collected comprehensively, and clinical procedures are not filed timely and accurately. Medical billing solutions can offer comprehensive data collection services for holistic data within a medical billing software. Electronic data interchange in medical billing can drastically reduce security breaches by collecting patient data and encrypting it toward medical billing codes. Finally, accurate and complete data erases the possibilities of duplicate claims, further delaying payment processing. Automated information filling, such as social security numbers, demographic codes, etc., can speed up the medical billing process and procedures.
5. Added Standardization: Integration of EDI in healthcare, with other practice management solutions, amalgamates all services related to patient experience, administrative, clinical, and electronic billing solutions. When healthcare providers deploy multiple and separate systems in the organization that cannot function in tandem, the result is common electronic billing mistakes. EHR should not be limited to administrative tasks and clinical processes but rather be integrated and even into the medical billing software. When medical billing solutions can pull out information from one standard system or platform, the possibilities of improper medical billing are diminished significantly. Information collected right from the stage of appointment scheduling up until the endpoint of bill generation keeps medical care functioning efficiently.
6. Reduced Carbon Footprint: This is one of the most underappreciated benefits of using EDI billing integration solution. By replacing multiple paper-based workflows with digital ones, an electronic billing platform significantly reduces the amount of paper. The bigger a medical organization gets, the more paper this software saves. Needless to say, this goes a long way in reducing the organization’s carbon footprint.
How Does EDI Work in Medical Billing Services?

Medical billing is a complex and time-consuming process that can be simplified by implementing Electronic Data Interchange (EDI) electronic billing services. These services streamline the process by reducing manual processes and ensuring proper coded procedures, diagnoses, and medical services.
The EDI billing process starts with an inquiry from the care provider and ends with a response from the payer. Each inquiry contains identifying information, such as the member ID number, date of birth, and payer ID. Requests can be sent directly to the payer or through a clearinghouse, which reformats claims and facilitates inquiries. When the inquiry is forwarded to the payer, they respond to the clearinghouse, who then sends the data to the care provider. Lastly, the response received can be a confirmation or a request to rectify the errors in the request and resubmit it to the clearinghouse.
Electronic bill payment service providers act as intermediaries between providers and payers, making the process convenient. EDI has gained widespread use in the healthcare industry as outsourcing medical billing services becomes more common.
How To Choose a Software For EDI Medical Billing
1. Check the Vendor’s Track Record
This is important when paying for a software platform for EDI in healthcare. Medical software is a large industry and still growing every year. That means numerous companies will offer a wide range of software applications for numerous purposes. So, an executive at a hospital would have to choose from many options, something that could become daunting. But an important factor that indicates the quality of an EDI billing platform is the company’s track record.
If the company has been in business for a decade or so and has a sizable presence in the market, it is usually a promising sign. It indicates a steady clientele and quality products, not to mention competent leadership. It would be even better if you could personally view the company’s software at a hospital or an insurance payer organization to see for yourself.
2. Support
The ability of the vendor to provide support is also a major deciding factor when purchasing software for EDI in medical billing. Glitches, downtimes, and other problems would cause hospital billing operations to come to a standstill. During such times, timely support would ensure business continuity and prevent operational problems for the organization.
The type of support also offered matters. On-site technical support would be preferable in case of major problems, while online support is suitable for smaller issues. Nevertheless, the ability of a vendor to provide support when needed is an important consideration when buying a medical billing solution.
3. Staff Training
Once the EDI healthcare solution has been implemented, the vendor must provide training for the staff at the organization where it is deployed. This training must be comprehensive and enable the staff to carry on operations without hassle. Implementing a medical EDI system is to streamline all the activities surrounding medical billing, so staff must be able to operate the platform naturally.
4. Scalability
A medical organization might grow in size and the services provided. This means it would have to incorporate newer workflows, processes, and protocols regarding billing activities. So, a platform for carrying out a medical billing process at a hospital or clinic would need to accommodate features for additional processes as the organization grows. This could mean more features and more instances of the EDI billing software.
When a hospital or clinic purchases a medical billing platform, it must ensure that the solution can accommodate growth. Otherwise, the organization would have to purchase whole new software, which would cost time and money. On the other hand, if the vendor can add more features as the client’s need evolves, it would go a long way in enabling the vendor to maintain a steady clientele and the hospital to serve its patients well.
Trends in Healthcare EDI Billing
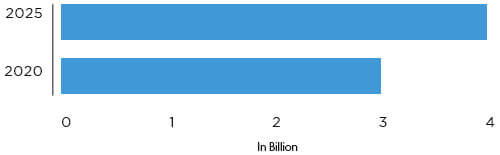
The global healthcare EDI market, valued at $3.0 billion in 2020, is expected to reach $4.4 billion by 2025 due to its increased security, accuracy, efficiency, and standardized communication. EDI in healthcare secures the exchange of sensitive data quickly in a standardized format, reducing processing delays and maintaining HIPAA compliance through the ASC X12 protocol. It also improves processing efficiency by automating administrative tasks in claims processing, such as claim transmission and payment tracking.
EDI is becoming the standard in medical billing, allowing for easy data exchange in medical facilities. The current EDI trends that medical institutions are already leveraging include the ePCR System, which ensures legible and accurate patient care reporting, and blockchain technology, which promises secure and private transactions.
Additionally, AI is also being used in healthcare institutions to diagnose several illnesses in patients and recommend suitable treatment plans, demonstrating the potential for AI to become a more advanced tool in the healthcare industry. Overall, these trends are transforming the way medical facilities operate and communicate.
Myths About Healthcare EDI
APIs are Better for Small Practices
While it is commonly assumed that EDIs are only suitable for large hospitals, they are also suitable for small medical practices. Software for EDI in healthcare can be easily integrated into existing systems at practices and offers a secure exchange of sensitive data for small practices.
EDI Solutions Are Not Secure Enough
This is another common myth associated with healthcare EDI billing software. The platform complies with HIPAA regulations and ensures a high degree of security for the data exchanged. It includes protocols and features that prevent data leakage and protect its integrity.
An EDI Will be a Risky Investment
Many providers, especially at small practices, believe that investing in an electronic billing platform might be too big an investment and won’t provide adequate returns. This primarily stems from the fact that a medical EDI depends on the value-added network (VAN) to deliver messages. But what is to be noted is that an EDI automates many aspects of handling data during interchanges, which eventually reduces the average cost per transaction. It will deliver returns in the long run.
Cost to Set Up EDI

EDI billing cost usually depends on the approach and the selected procedure. There are primarily two options available: one is to use an in-house licensing model, where the business acquires the hardware and software and installs them on the premises. This solution costs anything from a few hundred dollars to a few thousand, depending on the level of support required during the installation and maintenance.
The second option is using a subscription model, which involves subscribing to a trading partner and using a SaaS or cloud-based EDI solution provider. The cost of this approach depends on the level of support and the number of trading partners. The volume of transactions can also play an integral role in determining the cost, as some providers charge based on the transactions.
Overall, EDI billing services are a valuable tool for businesses looking to streamline their billing and payment processes. They offer faster, more efficient, reliable, and secure ways of exchanging billing information, helping medical institutions improve cash flow and reduce the risk of errors and fraud.
Conclusion
Keeping in mind the points mentioned above, it is most advisable to adopt an advanced EDI billing software solutions with automated features when it comes to medical billing. This will ensure that medical billing mistakes, coding errors, incorrect information, and cash flow delays are explicitly avoided. Medical bills are double-checked before being submitted to insurance carriers, and there is no duplication of data entry. Fewer denied and rejected claims, reduced workload for staff, fewer pending claims, increased overall profits, and higher patient satisfaction are all attainable factors with the right kind of EDI billing software systems.
The software industry has been growing steadily over the last decade. As newer technologies emerge, it becomes increasingly important for stakeholders to adopt them to stay relevant. Implementing EDI billing solutions is no longer an option but necessary for the oncoming technological transformation. If you are looking for best-in-class EDI billing solutions for your healthcare organization, get in touch with our experts.
The industry software technology has constantly been growing since the last decade. As newer technologies emerge, it becomes increasingly important for stakeholders to adopt them to stay relevant. Implementing an EDI billing solution is no longer an option but necessary for the oncoming technological transformation.
OSP is a trusted healthcare software development company that delivers bespoke solutions as per your business needs. Connect with us to hire the best talents in the industry to build enterprise-grade software.

How can we help?
Fill out the short form below or call us at (888) 846-5382
Discuss Your Project Handover with a team of expert Book a free consultation arrow_forward
About Author

Written by Riken Shah linkedin
Riken's work motto is to help healthcare providers use technological advancements to make healthcare easily accessible to all stakeholders, from providers to patients. Under his leadership and guidance, OSP Labs has successfully developed over 600 customized software solutions for 200+ healthcare clients across continents.